Is Proton Beam Therapy More Effective Than Traditional Radiation
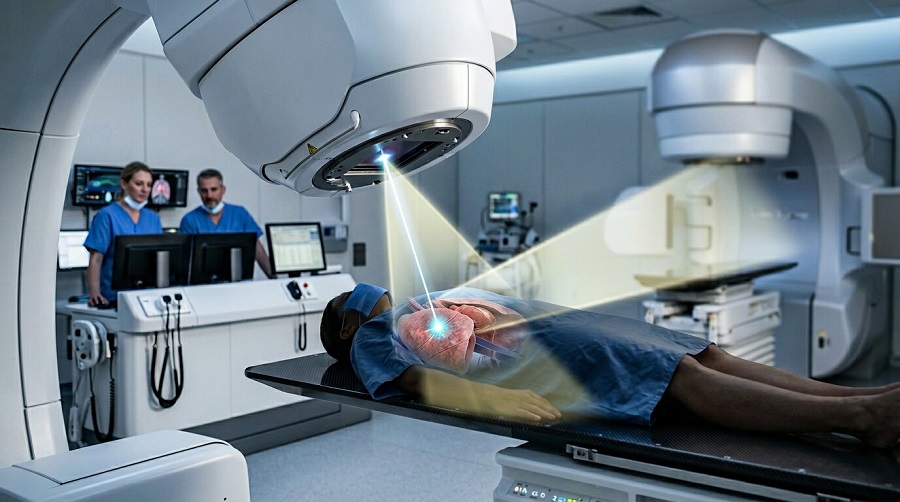
When you’re weighing proton beam therapy against traditional X-ray radiation, you’re really asking two questions: will it control your cancer just as well, and will you feel better during and after treatment? Current studies suggest proton therapy can match X-rays for survival and cancer control, while causing fewer serious early side effects. But before you assume it’s automatically the better choice, you’ll want to look closely at one crucial limitation in the evidence so far.
Proton vs X-Ray Radiation: Which Is Better for You?
When comparing proton therapy with traditional X-ray (photon) radiation, the question is rarely about which is universally “better,” but rather which is better suited to a specific patient, tumor location, and overall health profile. In many cases of non-metastatic cancers, both approaches yield similar outcomes in tumor control and overall survival, with studies showing comparable 3-year cancer-free and overall survival rates.
The difference becomes more meaningful in how each treatment affects the body during and after therapy. Proton therapy is designed to deliver radiation more precisely, limiting exposure to surrounding healthy tissue. This often translates into fewer severe side effects. Some large studies report significantly lower rates of complications requiring hospitalization compared to traditional X-ray radiation. Patients undergoing proton therapy have also shown fewer declines in daily functioning, even among those who are older or managing additional health conditions.
This is why working with a team that understands both advanced treatment options and the nuances of your local healthcare landscape matters. Access to specialized care, coordination with nearby providers, and familiarity with regional treatment centers can all shape the experience and outcome. For example, exploring proton beam therapy for lung cancer with a provider experienced in both modalities can help determine whether the precision benefits of protons are meaningful for your specific tumor location, particularly when protecting nearby organs such as the heart or lungs is a priority.
The right choice depends on a careful balance of clinical evidence, individual health factors, and access to experienced providers who can guide treatment decisions with both expertise and context.
How Proton Therapy Works Differently From X-Ray Radiation
Understanding how proton therapy behaves inside the body helps clarify why its side‑effect profile can differ from traditional X-ray radiation. In proton therapy, a beam of positively charged particles is directed at the tumor. These particles deposit relatively little energy at first, then release most of their energy at a specific depth (the Bragg peak) and then stop. This creates a sharp dose fall-off beyond the target, which can reduce radiation exposure to tissues beyond the tumor.
X‑ray beams, by contrast, deposit radiation continuously along their path as they enter the body, pass through the tumor, and exit. As a result, both tissues in front of and behind the tumor receive a dose.
Proton therapy planning uses detailed imaging and three‑dimensional dose calculations, often with repeated verification scans, to align the high‑dose region with the tumor as accurately as possible and account for factors such as patient positioning and organ motion.
Does Proton Therapy Control Cancer as Well?
Available evidence suggests that proton therapy and traditional X‑ray (photon) radiation provide broadly similar cancer control in many non‑metastatic cancers.
In a large, non‑randomized study of patients with non‑metastatic disease, three‑year cancer‑free rates were 46% with proton therapy and 49% with X‑ray radiation.
Overall survival at three years was also similar: 56% for proton therapy and 58% for X‑ray treatment.
At one year, cancer control and survival outcomes were again closely aligned: 83% for proton therapy and 81% for X‑ray radiation, with no statistically meaningful difference between the two groups.
Because this comparison wasn't based on a randomized trial, it can't definitively establish that proton therapy and X‑ray therapy are equally effective.
However, within the limits of observational data, the results indicate that cancer control and survival outcomes appear broadly comparable between the two approaches in this setting.
Side Effects: Proton Therapy vs Traditional Radiation
Although proton therapy and traditional X‑ray radiation achieve similar cancer control, they differ in how often they cause serious short‑term side effects. In a large observational study, about 12% of people receiving proton therapy experienced severe side effects within 90 days, compared with 28% of those treated with traditional radiation.
Patients receiving proton therapy were also less likely to experience a decline in day‑to‑day functioning; decreases in performance status occurred at roughly half the rate observed with traditional radiation, despite the proton therapy group being, on average, older and having more health problems. The study also found fewer unplanned hospitalizations and emergency department visits among people treated with proton therapy.
Because the study was observational rather than randomized, these findings indicate an association rather than definitive proof that proton therapy causes fewer side effects. Other factors, such as differences in patient selection, treatment planning, or supportive care, could have influenced the results.
Costs, Insurance, and Access to Proton Therapy
While proton therapy may reduce severe side effects and unplanned hospital visits compared with conventional radiation, it's associated with higher upfront treatment costs and variable insurance coverage.
Insurers often apply stricter review criteria, citing limited randomized data to justify the added expense, especially for some cancer types.
Observational studies suggest that patients receiving proton therapy experience fewer severe side effects, about 12% versus 28% within 90 days in one analysis, which can lead to fewer hospitalizations and emergency department visits.
When these downstream medical costs and potential improvements in quality of life are considered, overall expenses may be closer to those of conventional radiation, although this can vary by patient and cancer type.
Several randomized clinical trials are underway and may provide more definitive evidence on clinical benefits and cost-effectiveness, which could influence future insurance coverage and availability.
Conclusion
When you compare proton beam therapy with traditional X-ray radiation, you’re usually looking at similar cancer control but different side‑effect profiles. Proton therapy may lower your risk of serious early complications, but it’s not clearly superior for survival, and access and cost can be challenging. Talk with your oncology team about your specific cancer, other health conditions, insurance, and location so you can choose the option that best fits your needs and priorities.
